When Burnout Meets cPTSD: The Quiet Slide from Overdrive to Shutdown
Maegan Bradshaw, March 31, 2026
Have you ever been the person who can handle everything… until suddenly you can’t?
You’re the one who shows up.
Who solves problems.
Who keeps things moving even when everything feels chaotic.
And then one day your brain feels foggy. Your body feels heavy. Simple tasks feel strangely difficult.
You might wonder:
Am I depressed?
Am I just exhausted?
What happened to the version of me who always powered through?
For many people living with complex PTSD (cPTSD), what’s happening isn’t always depression or laziness or a lack of motivation.
Sometimes it’s your nervous system shifting gears.
And when burnout overlaps with trauma, that shift can feel confusing, frustrating, and deeply unsettling.

A Nervous System That Learned to Stay Alert
People who live with cPTSD often have nervous systems that adapted to environments where safety wasn’t consistent.
When the brain experiences chronic stress or trauma, the amygdala (the part of the brain responsible for detecting threat) becomes highly sensitive. It gets very good at scanning for danger.
At the same time, the prefrontal cortex (the part of the brain responsible for reasoning and regulation) has to work overtime to keep everything functioning.
The result?
A nervous system that lives in hyperarousal.
Hyperarousal is the state where the body stays on high alert. The sympathetic nervous system (the “fight or flight” system) is activated more often than it needs to be.
This can show up as:
• Anxiety or restlessness
• Racing thoughts
• Difficulty relaxing
• Irritability
• Trouble sleeping
• Feeling like you always have to stay “on”
For many trauma survivors, this state becomes normal. In fact, it can even look like high functioning.
You might become the person who handles crisis well. The one who anticipates problems before they happen. The one who keeps moving even when you’re exhausted.
Your nervous system learned: staying alert keeps us safe.
And for a long time, it works.
Until it doesn’t.
When Burnout Enters the Picture
Burnout happens when stress isn’t just intense; it’s chronic. It happens when the demands placed on us consistently exceed the resources, we have available to meet them.
When the demands placed on your mind, body, and emotional capacity continue for too long without enough rest, support, or recovery.
For advocates, caregivers, and people in helping professions, burnout often sneaks in quietly.
You care deeply about the work.
You know people are relying on you.
You push through hard days because the work matters.
Until one day your nervous system simply… can’t.
A nervous system that already runs in high alert has a smaller margin before exhaustion sets in. Eventually, the system has to compensate. Instead of just feeling tired or overwhelmed, the body can shift states entirely.

The Nervous System’s “Brake Pedal”: Hypoarousal
When the nervous system can’t maintain hyperarousal anymore, it may shift into hypoarousal.
Instead of fight-or-flight, the body moves into a shutdown state.
This response is connected to the dorsal vagal branch of the vagus nerve, part of the parasympathetic nervous system that slows everything down when the brain perceives overwhelming stress.
If hyperarousal is the nervous system pressing the gas pedal…
Hypoarousal is slamming the brakes.
This can feel like:
• Emotional numbness
• Brain fog
• Difficulty concentrating
• Low motivation
• Feeling disconnected from people or surroundings
• Extreme fatigue that sleep doesn’t fully fix
The nervous system isn’t trying to sabotage you.
It’s trying to protect you from overload.
For people with cPTSD, this shift can feel confusing and scary. You may have spent years being the person who could push through anything. Suddenly, you can’t. Things that used to feel manageable now feel impossible. Even simple tasks start to feel overwhelming.
Why This Can Look Like Depression
One of the most confusing parts of this shift is that hypoarousal can closely mimic depression.
From the outside (and sometimes even to ourselves) it can look like:
• Low energy
• Loss of interest
• Withdrawal from others
• Difficulty focusing
• Feeling heavy or slowed down
And sometimes depression is part of the picture.
But for many people with trauma histories, what’s actually happening is that the nervous system has reached a point where it simply can’t sustain high alert anymore.
Your body is not failing you.
It is trying to survive.
Your body is conserving energy after running in survival mode for a very long time.
Identity Whiplash: The Grief of Not Being the “High-Functioning” Version of Yourself
One of the hardest parts of this shift is the internal narrative that comes with it.
If you’ve spent years being capable, resilient, and productive (even under immense stress), entering a hypoaroused state can feel like losing your sense of self.
You might hear thoughts like:
Why can’t I just push through this?
I used to handle so much more than this.
What is wrong with me?
But from a nervous system perspective, the answer may actually be:
Nothing is wrong with you.
Your system has simply reached a point where it needs something different.
Not more pushing.... but more regulation, recovery, and safety.
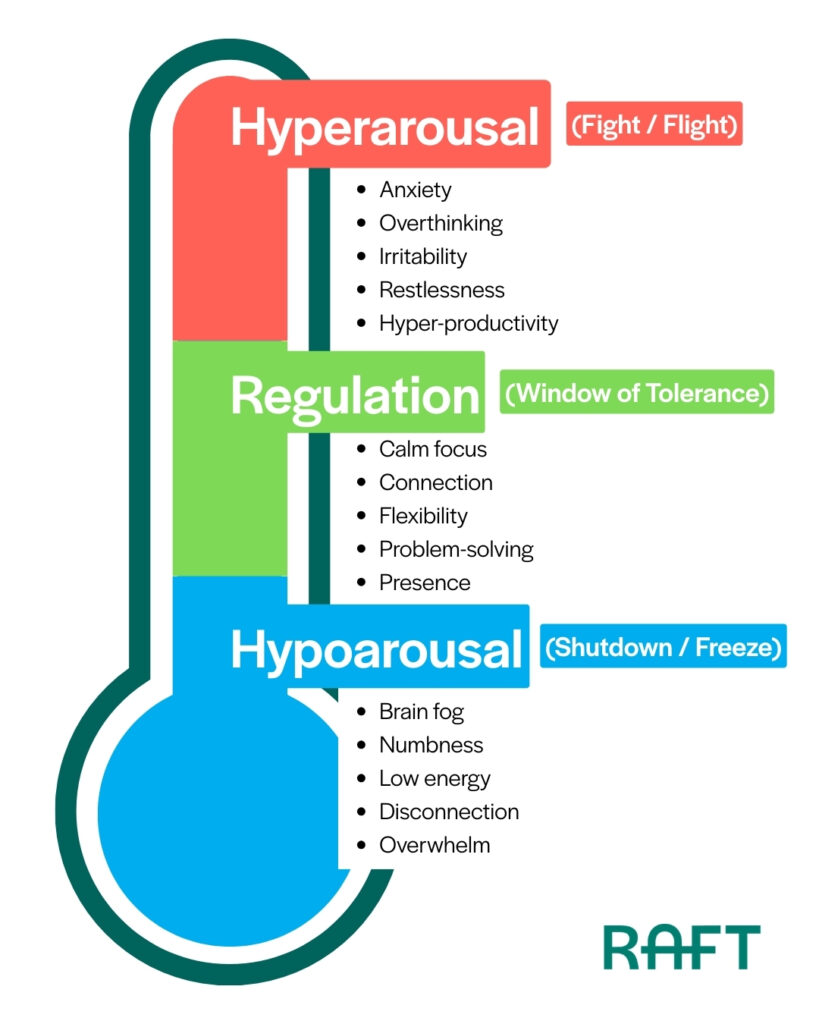
Moving Back Toward Regulation
The goal isn’t to force yourself back into hyperarousal. That’s the survival mode many people are trying to move away from.
Instead, healing often happens in what nervous system researchers call the “window of tolerance.” This is the zone where the nervous system is alert enough to engage with the world but regulated enough to feel safe.
When someone is in hypoarousal, the most helpful strategies are often gentle activation, not pressure. Small, manageable steps that slowly re-engage the nervous system.
Things like:
• Small movement – stretching, walking, or light activity
• Safe connection – brief conversations with supportive people
• Reducing overwhelm – focusing on one small task at a time
• Celebrating tiny wins – rebuilding momentum slowly
• Practicing nervous system awareness – noticing what helps you feel slightly more present or energized
Healing doesn’t usually happen through pushing harder.
More often, it happens through learning how to listen to the nervous system in new ways.
Naming It Matters
One of the most powerful things we can do, especially in advocacy spaces, is name what’s happening.
When burnout and trauma overlap, the experience can feel deeply personal, like something is wrong with us. But often, what we’re experiencing is a nervous system that has been working incredibly hard to protect us.
Understanding that shift, from hyperarousal to hypoarousal, can bring relief. Because the story changes.
Instead of:
Why can’t I keep up anymore?
It becomes:
My nervous system has been carrying a lot for a long time.
And that understanding opens the door for something new.
Not just surviving. But slowly learning what safety, regulation, and restoration can feel like.
A Gentle Next Step
If you’re recognizing yourself in this, pause for a moment.
Take one slow breath.
You don’t need to fix your nervous system today. You don’t need to push harder.
You might simply start by noticing:
What state am I in right now?
What would feel slightly more steady?
Sometimes regulation begins with something small. It’s as simple as stepping outside, softening your expectations for the day, or connecting with someone who feels safe.
And if these patterns feel persistent or overwhelming, additional support (including a trained therapist in this area) can be a powerful part of healing.
Awareness is not the end of the story. It’s the beginning of responding differently.
And responding differently is how sustainability starts.
Learn More About These Concepts
Understanding trauma and the body
The Body Keeps Score | Bessel van der Kolk
How the body keeps the score on trauma | Bessel van der Kolk for Big Think+
The Science & Biology of PTSD | PTSDuk
Nervous system states and regulation (Polyvagal Theory)
Using the Polyvagal Theory for Trauma | Dr. Stephen Porges, Being Well Podcast
Polyvagal Theory Made Simple | Mind Known
The Window of Tolerance explained
How to Help a Client Come Back into Their Window of Tolerance | nicabm
Window of Tolerance Info Sheet | John Hopkins University
The Window of Tolerance and PTSD | PTSDuk
Burnout and workplace stress
Burnt Out? | What Does Workplace Stress Do To My Body | National Geographic
Speaking of Psychology: Why we’re burned out and what to do about it | Christina Maslach, PhD







